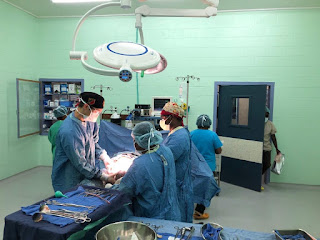
I wanted to share a few stories of patients I have taken care of while here. These are by no means representative of the people here, or even necessarily my work here, but rather stories that have touched my heart in one way or another.
My second day out of quarantine I did my first C-section here in PNG. The patient’s name was Karen, and she was 30 weeks pregnant with twins. She had been hospitalized over a week before due to severe preeclampsia (a condition in pregnancy where the blood pressure goes up, the kidneys spill protein into the urine). She had been treated with steroids to help her babies mature faster so that they would be ready for a premature exit and treated for her high blood pressures, but that day her blood pressures were not responding to treatment and the team was worried that she might develop seizures or other serious complications from preeclampsia.
The first twin was in a breech position where the legs and butt are down instead of the head, so the decision was made to proceed with a C-section. Not having done a C-Section for about 7 months since the end of residency I was nervous heading into the surgery. As we prayed for Karen before starting the case, I tried to take a few deep breaths to steady my hands, and my prayer took on a greater sincerity. Dr Ben, the general surgeon at the hospital, was my overqualified assistant and helped me orient to doing surgery here. Thankfully the surgery went well and both babies were delivered safely.
A few weeks later I returned to work on our OB Ward. To my delight, I was able to resume care for Karen and her two babies, a boy and a girl. Over the next several weeks I was able to watch them grow, learn how to breast feed, no longer require the NG tubes (tubes through the nose into the stomach used for feeding) or the oxygen. This last weekend they had both made it past 2kg and were growing well by just breastfeeding. I was able to send them home. It was a bittersweet departure, joyful at their progress and ability to go back home but also sadness that I would not be able to see these twins grow and see Karen’s shy smile every morning.
……
I was convinced that Bill would not survive when I saw his mother carrying him into the emergency room. She was trying to breathe into his mouth while carrying him in, a sign that he was not breathing. I rushed over with the nurse and helped her lay him on a patient bed. Amazingly he still had a pulse, but he was not taking any breaths on his own. We started using a bag-mask to help him breathe while the nurse took vital signs and attempted to get an IV. His mother stated that he had been having bad diarrhea for weeks. After 5 minutes he began to take breaths on his own and after 10 minutes he no longer needed our support to breathe, just some oxygen. We were unable to get an IV so I had to place an IO-a needle that goes into the marrow of the bone to allow us to give fluids.
That night I walked up to the hospital two more times to check on him, each time a little surprised but also thankful that he was still alive. That night I prayed, trying to trust Bill to God. In my work here and in Malawi I have seen many kids die. Sometimes they came in like Bill, malnourished and dehydrated on the verge of collapse, only to die within a few minutes of arriving despite our attempts. Others suffering from malaria or trauma or premature birth would last a little while longer only to succumb to the overwhelming pathology. But thankfully, by God’s grace, his attentive mother and the nursing staff, he not only made it through that night but also the next one and the next one.
I checked on Bill several times over the next few days, every time seeing him more alert and interactive. A week after he was brought in, I took this picture.
Seeing children die can be overwhelming, heartbreaking and discouraging. But thankfully we are able to make a difference for many. And for Bill that difference means the world.
….
Rose was brought into our hospital by a helicopter from the Jimi valley, a large valley north of our hospital, that despite not being a long distance away (40-60km), can present an often-insurmountable barrier to access for our patients that live there. With a reliable car, it is a 4-5 hour very bumpy ride out to our small health outpost in the Jimi Valley. For many of our patients it can be a trip of several days. Luckily for Rose, she was able to be brought in by a helicopter for obstructed labor.
Rose had been in labor for 2 days but had not been able to deliver her infant vaginally. Our hospital is the only health care facility for our province of 350-400,000 people that has surgical capabilities and can provide blood products. As such, we see a large number of complicated obstetrical cases.
We brought Rose back quickly for a C-Section. The baby was difficult to extract due to the length of her obstructed labor and the moulding of the head into the pelvis. There was thick meconium (baby poop) that had obviously been present for some time. Thankfully Dr Ben was available to help me with the delivery. I scrubbed out of the case to help resuscitate the baby while Dr Ben started to close the uterus. After about 10 minutes of resuscitation the baby was crying and breathing on its own.
Over the next few weeks, I have been able to care for Rose and her baby. Rose initially healed very well; however, she subsequently developed a wound infection and has required further care and antibiotics in the hospital. As she is not able to get wound care near her home in the Jimi Valley, we have kept her here to continue to help her heal in a safe environment. Her baby has done very well and seems to get bigger every day.
Every morning Rose greets me with a soft, shy smile. She has been so patient throughout her time here. I am so glad that she was able to arrive when she did. If she hadn’t and if this hospital weren’t here, both her and the baby likely would have died.
I hope these stories encourage you as much as they have encouraged me. Sometimes seeing the health disparities here can be discouraging, but there are bright lights like Karen, Bill and Rose too that give me strength to keep working to help the people here. I am so thankful for the staff here who have been giving of their lives to help this community for years and years.
I would really appreciate your continued prayers. We are in the midst of our first large outbreak of Covid in the province and there is a lot of fear and uncertainty. Many patients are not coming into the hospital due to this fear and we know that this is probably leading to a number of patients, especially pregnant women, not receiving critical care. I’d also appreciate prayers for finding community amidst a pandemic and perseverance as I continue to have so much to learn, language, culture, tropical medicine and especially learning to make diagnoses/decisions in the face of uncertainty.
I want to end with a Henri Nouwen quote from a devotion today, “Learn the discipline of being surprised not by suffering but by joy. As we grow old…there is suffering ahead of us, immense suffering, a suffering that will continue to tempt us to think that we have chosen the wrong road…But don’t be surprised by pain. Be surprised by joy, be surprised by the little flower that shows its beauty in the midst of a barren desert, and be surprised by the immense healing power that keeps bursting forth like springs of fresh water from the depth of our pain.”
You all are in my prayers. I love hearing from you!